Pubs and restaurants welcomed streams of people through their doors over the summer, so why was becoming a mother made to be a more emotional journey of pregnancy, with people experiencing labour and birth alone? Here, Mari Ellis Dunning reflects on becoming a mother during a global pandemic.
(Note: This article was written at the end of October 2020, just as Wales entered a second national lockdown)
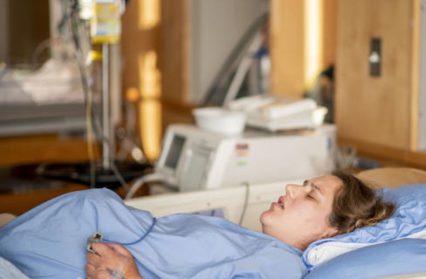
Image Credit: FatCamera
The recent global pandemic caused by the novel Coronavirus, or COVID-19, has dramatically changed the lives of people all over the world. Since March, we’ve been trapped indoors, unable to socialise with our closest friends and family for months, to travel outside of our local communities at times, or even to spend any significant amount of time outdoors without restriction.
I think back now to the early summer months of the global pandemic. As I was becoming a mother, this time is particularly challenging for me – I face the second and third trimesters of my pregnancy in isolation, unable to seek support from those I am so desperate to spend time with – my mother, my sisters, my best friends. Instead, I lie in the back garden under a baking summer sun, watching my watermelon belly move as the baby squirms inside me. He flips and rolls. He kicks. I capture these movements on my phone camera, send videos to everyone I think will be interested. As I marvel at this little bean’s movements, it tugs at me that no one but my husband can rest a hand on my stomach and share at this moment which I find nothing short of miraculous.
Four weeks before my son is due, my waters begin to leak. I drive myself to the hospital, not overly concerned, since I’ve been experiencing mild contractions for a few weeks already, and expect to be told that I am in latent labour and that my baby will come when he is ready. After a few hours sitting alone in the waiting room, I am taken into the antenatal ward, where I am strapped to a machine that monitors foetal movement, and the waters are assessed. They tell me that I am, as I suspected, in early labour. I expect I’ll be allowed to go home, to continue as I have been until the baby is more properly on his way, but they tell me that this isn’t an option. They tell me that I must go to a different hospital, an hour away from home, where the facilities for premature births are better. I had been dreading this, had been silently begging the baby to stay put for another week so that I could have him at my local hospital, close to home and in the award, I am familiar with. I contact my husband, who works in the hospital’s Medical Assessment Unit and meet him in the corridor where I rest my head on his chest and cry, realising that we will be parents very soon, whether or not we feel ready.
In the ambulance (which I am adamant I don’t need but am made to ride in as a precaution), the contractions become stronger. It’s almost as though I’ve given my body permission to begin labour, or given my baby permission to begin his journey, now that the hospital has confirmed what I have suspected for weeks. When we arrive at the other hospital, I am nervous. My planned midwife-led delivery, involving a birthing pool, low lighting, candles and music, has been replaced by the stark reality of a brightly lit ward, unfamiliar faces half-hidden behind masks, and the smell of antiseptic.
My husband, who has stopped at home to collect my overnight bag, meets me at the door to the ward and hands over my things. I let him hold me for a brief moment, knowing that the next time we see each other will be when I am deemed by hospital staff to be in ‘active labour’, which could be in as little as a few hours time, or as far away as a few weeks. Oxytocin and endorphins are natural painkillers known to ease the transition between the latent stage and first stage of labour; in other words, the support of a loved one can help a woman to move from the early stages to active labour much more comfortably and quickly.
Despite this, I spend the night alone, labouring slowly and steadily throughout, trying to focus on the positive affirmations I have practised, and stave off any fear about delivering a premature baby and the complications this could entail. I keep in touch with my friends via our Facebook group chat, updating them on the progress of the surges. I watch Netflix on my phone screen and listen to trolleys moving up and down the corridor, eliciting a sound reminiscent of ‘The Wheelers’ from the 1985 movie Return to Oz. I don’t sleep, not even for a moment.

The next morning, my waters break fully. The surges become too powerful and regular for me to keep in contact with anyone, so my phone is put away. I try to butter a slice of toast someone has brought and left beside the bed, knowing I’ll need the energy, but I can barely take a bite before another surge begins. I am left like this for hours, entirely alone except for a midwife who occasionally pops in to make brief observations. I never see more than half of her face – her smile is hidden by the fabric. I am told my husband cannot join me until I am moved to the Labour Ward, so I allow the midwife to perform an internal examination. Despite my resolution to avoid any IEs, I know I will be moved more quickly if the medical team can determine that I am 4cm dilated (an arbitrary measurement which amounts to absolutely nothing in regards to how labour will progress), and at this point, my desire to have somebody, anybody, at my side far outweighs my previous reluctance to have a hand thrust into my cervix between intense surges.
When he slips into the world, my son is a decent weight – 6lbs and 5oz at four weeks early. Nonetheless, a few complications related to his preterm birth mean that he has to stay in the Special Care Baby Unit (SCBU) for a week, while I stay on the postnatal ward to be near him. This means a week in hospital with no visitors – no family, no friends, and no one allowed to meet my son. No one to hold my hand while I weep with exhaustion. Again, I send photos and videos, chat to friends using FaceTime, trying to find quiet corners where I can do this without being overheard.
My husband is able to visit our baby in SCBU, but only by himself – despite living together, we can’t be on the ward at the same time, can’t bond with our baby together, can’t support each other in this difficult and frightening time while our tiny baby is hooked up to machines and tube fed because he is too tired to coordinate breastfeeding. At my insistence, I am able to attempt to feed him myself before he is ‘topped up’ through a nasogastric tube, but this means that my husband’s visits with his newborn son are cut short – for me to enter and feed our baby, he must leave. I worry about this affecting his ability to bond. Only later do I learn that evidence does indeed show that infant bonding and attachment with parents increases in the periods around birth.
A handful of times, we coordinate meeting briefly in the corridors in what feels reminiscent of our school days, when we would touch each other’s hips in the hallways between classes. When we finally get home a week later, we make the difficult decision not to allow even my husband’s parents to hold our baby, at least not until he is a little bigger, a little more robust. He is their first grandchild.

Over the summer, the phrase ‘Eat Out to Help Out’ is plastered across social media, the government and the tourism industry encouraging us to dine out for the sake of ‘the economy’. Meanwhile, for pregnant women and new mothers in the UK, the difficulties are only increasing. The guidelines and regulations, although supposedly designed to protect us, are unjust. While groups can now freely meet in bars and restaurants and are in fact actively encouraged to do so for the sake of ‘the economy’, pregnant women are still having to attend ultrasound scans alone, potentially to learn that their baby is suffering from complications, or even that their baby has no heartbeat. They are forced to labour alone on antenatal wards with no birthing partners at their sides. Those same birthing partners could, however, be downing a pint at their local, amongst hoards of other people.
During this time, a friend gives birth to her second child. Her husband rushes into the room as the baby’s head is crowning, nearly missing the birth entirely. Another friend sits alone on a theatre bed, about to undergo an unplanned caesarean section. The midwife holds her hand as she cries. A clear example of how becoming a mother during a pandemic was so difficult.
Post-birth, there are no cups of tea with health visitors, no routine postnatal checks to ensure women are healing physically and mentally, and no opportunities to socialise with other new or expecting parents. While I have been navigating motherhood alone, pacing the living room and wondering when my friends might be able to meet my child, large groups have continued to meet in pubs across the UK, or drunkenly gathered outside of nightclubs. This, we are reminded, is good for ‘the economy’.
It’s drawing close to Halloween now, the country has entered a National Lockdown, and still, no one outside of our immediate circle has been able to cuddle or enjoy our little boy as he reaches four months old. This second lockdown comes as a result of a predictable ‘second wave’, buoyed perhaps by the summer’s insistence on ‘Eating Out’ and ‘Helping Out’. In Wales, there is uproar as shops are instructed to sell ‘essential goods only’ for the duration of the two weeks Firebreak Lockdown. There is widespread anger, there are protests, there are petitions which reach over 67,000 signatures in less than a week. A man enters Tesco in only his underwear in protest; shoppers tear down tape covering ‘non-essential’ items; within days, the Welsh government relents, leaving shops to deem items ‘essential’ or not at their own discretion. Meanwhile, for women frantically searching an ultrasound for a heartbeat, pacing an antenatal ward alone, or sitting at their premature baby’s incubator, there are no riots. A petition collects just over 7,000 signatures. Nothing changes.
Another piece, similar to this Becoming a Mother During a Global Pandemic piece by Mari Ellis Dunning for Wales Arts Review is also available to read.
A similar piece surrounding the repercussions of Covid-19 is available to read also.










